Key Takeaways
- Embryo grades describe how embryos look and grow in the lab, not your guaranteed chances of pregnancy.
- You do not need to decode every letter and number on your own. It’s okay to ask, “Which embryos are you most hopeful about, and why?”
- Even “okay” or “lower” grades can still lead to healthy pregnancies and babies.
- Doctors and embryologists look at much more than the grade when planning your transfer, including your age, medical history, and overall treatment plan.
- Joy of Life is here to help you understand the reports you receive and prepare good questions for your clinic, so you never feel like you’re reading them alone.
When you’re going through IVF as part of your surrogacy journey, you’ll eventually hear about embryo grading.
On paper, it can look intimidating — numbers, letters, and charts that seem to say a lot about your future in just a few characters. In reality, embryo grading is simply a way for the lab to describe how embryos are growing so they can decide which ones to try first. It is not a promise of success or a judgment about what kind of child you’ll have.
You don’t have to become an expert in lab terminology to move forward. Your clinic and the team here at Joy of Life can help translate those grades into clear, calm guidance so you feel informed, hopeful and supported.
Why Embryo Grading Charts Exist
Clinically, embryo grading is a non-invasive visual assessment that embryologists use to score an embryo’s development based on its appearance under the microscope (its morphology). In everyday IVF practice, this means that over the first few days after fertilization, an embryologist checks each embryo under a microscope and records its development at each point in time.
The goal is to answer questions like:
- Are the embryos growing at a healthy pace?
- Do the cells look the way we expect them to at this stage?
- Which embryos should we consider transferring first?
A few important clarifications:
- Embryo grading is not a genetic test. It shows how an embryo looks and grows, not whether its chromosomes are typical or whether it carries specific genetic conditions.
- It is not a guarantee of pregnancy or birth. A “top” grade cannot promise a certain outcome, and a “fair” grade does not mean an embryo has no chance.
- It does not predict your child’s personality, abilities, or who they will become. It’s a snapshot in the lab, not a crystal ball.
You may also hear about PGT-A (preimplantation genetic testing for aneuploidy). This is a separate process in which a small sample of cells from an embryo is tested to see whether it has the expected number of chromosomes. PGT-A often leads to terms like “euploid” (chromosome count looks typical) and “aneuploid” (extra or missing chromosomes). That’s different from visual grading, though both can be used together when doctors are planning which embryos to transfer.
At every step, we can help you:
- Understand what your clinic’s reports are saying in simple language
- Prepare questions before your appointments
- Feel more grounded when decisions about transfers are being made
5 Key Factors in Embryo Grading
Instead of memorizing every number and letter, focus on a few big ideas. Here are five key factors that actually matter when you’re looking at an embryo grading chart.
1. Embryo Development Stage (Where It Is in the Timeline)
Embryos undergo rapid changes in the first days after fertilization. Clinics usually check them at specific points in the IVF timeline. For example, a few days after fertilization and again as they reach the blastocyst stage (often around day 5 or 6).
The main idea:
- Earlier checks: Is the embryo dividing as expected?
- Later checks: Is it forming the structures we want to see before transfer?
You can think of it like checking in on a seed you’ve planted:
- Day 1: Is it in good soil and getting water?
- A bit later: Are the first little leaves starting to show?
Embryo grading is the lab’s way of confirming that growth is on track for each stage.
2. Cell Development Pattern (How the Cells Divide and Organize)
Another key factor is the embryo’s cell development pattern — how its cells divide and organize over time.
Healthy growth often looks like:
- Cells are dividing in a steady, organized way
- The embryo is keeping pace with where it should be in the timeline
The seed analogy works here, too. When you check your plant, you’re not counting every molecule; you’re noticing whether it looks healthy, steady, and on schedule for its age.
Even if an embryo is a little ahead or behind, what matters most is whether the overall pattern looks promising and stable.
3. Embryo Morphology (How It Looks Under the Microscope)
Embryologists also evaluate embryo morphology, which is the embryo’s overall appearance under the microscope. In medical language, this often includes looking at fragmentation, AKA, small bits of cell material that appear between cells, and how well the main structures are formed.
A more uniform, well-organized appearance is often considered a positive sign. But this is where it’s important to remember:
- Many less-than-perfect-looking embryos still lead to healthy pregnancies and babies.
- An embryo that looks a bit “irregular” in the lab can still have meaningful potential.
- The grade is one clue among many, not a verdict.
4. Embryo Grade Codes (What 3AA, 4BB and Similar Labels Mean)
Most embryo grading systems use shorthand grade codes that mix numbers and letters, such as “3AA” or “4BB.” Very simply:
- The number often describes how far the embryo has developed (for example, how expanded the blastocyst is).
- The letters usually describe the appearance of key parts of the embryo under the microscope.
Every clinic’s system is a little different, and they may use their own charts or scales. That’s why you don’t need to decode this alone.
The key idea is that these labels help your clinic decide which embryos to transfer first, not which embryos “deserve” to come to fruition.
Your doctor or coordinator can tell you, in plain language, which embryos they feel most hopeful about and how they plan to use the others in future steps.
A helpful question to ask is: “Based on these grades, which embryos are you most optimistic about, and what is the plan for the others?”
5. Overall Clinical Context (Why the Grade Alone Isn’t the Decision)
Perhaps the most important point of all is knowing that an embryo’s grade is only one part of the bigger clinical picture. Your clinic will also look at:
- Your age
- Your medical and fertility history
- Any past IVF or transfer outcomes
- Whether PGT-A or other testing has been done
- The overall number of embryos available
“Average” or “not perfect” grades can still be part of very successful IVF and surrogacy journeys. Many intended parents have ultimately welcomed healthy babies from embryos that were not considered “top” on paper.
The grade is a tool, not a verdict. What matters most is how your medical team uses all of this information together to build a thoughtful plan for you.
How Clinics Use Embryo Grades in Real Life
Once the lab has graded the embryos, your care team starts thinking about the order and timing for which embryos to transfer first and what to do with the rest. In everyday language, that might look like this:
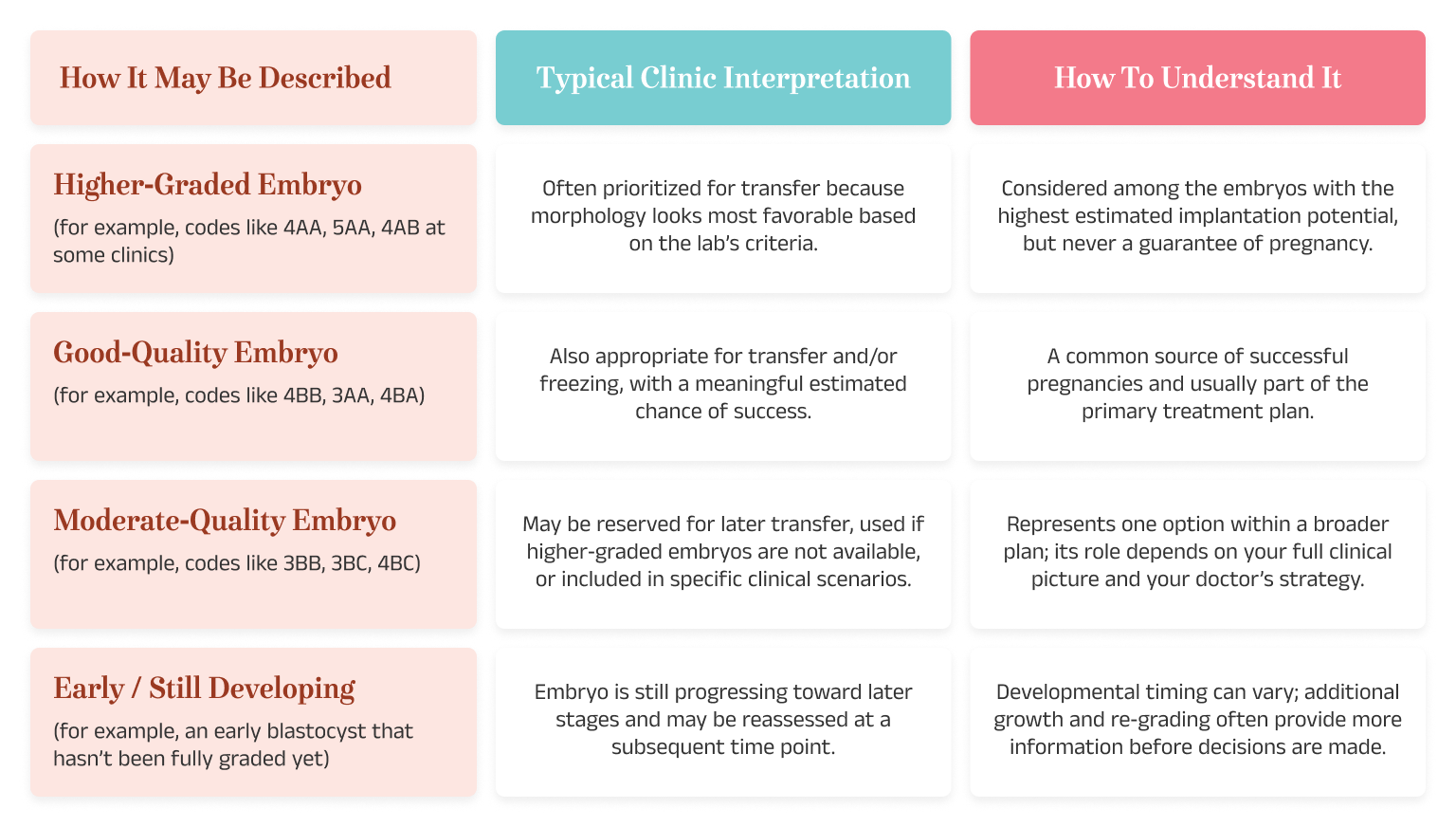
Note: Exact letter‑and‑number codes (such as 3AA or 4BB) and the cutoffs for each grade can vary by clinic and grading system. Your clinic can explain how their chart maps to “higher‑,” “good‑,” or “moderate‑quality” embryos in your specific case.
In practice, your care team will use embryo grades alongside your age, medical history and past treatment outcomes to help decide which embryos to transfer when and how to plan future steps.
If you ever feel lost in the terminology, you can always bring the conversation back to:
- “What does this mean for our next step?”
- “What are you recommending, and why?”
If you’d like support preparing for those conversations or understanding your options, you can get started today by scheduling a free consultation with our team at Joy of Life.
Frequently Asked Questions About Embryo Grading
1. Is a lower‑graded embryo still worth considering?
Yes. Embryo grades are probability guides, not verdicts. A lower-graded embryo may have a smaller chance of leading to pregnancy than a top-graded one, but:
- Lower-graded embryos do implant and develop into healthy pregnancies.
- Many families have children today from embryos that were not the “best” option on paper.
If your clinic recommends or includes a lower-graded embryo in your plan, it’s because they still see meaningful potential for it within the full clinical picture, not because you are “out of options.”
2. Do I have to understand every code on my report?
You don’t. It’s perfectly okay if the letters and numbers never fully “click” for you. What matters is that you:
- Understand the big picture of what your doctor is recommending
- Feel comfortable asking questions until the plan makes sense
A simple, powerful question to use is, “Which embryos are you most hopeful about, and why?”
From there, your clinic can walk you through the reasoning in language that feels more manageable, and your Joy of Life team can help you revisit that explanation later if you need to hear it again.
3. Why do different clinics explain grades differently?
Every clinic has its own style and system. Some:
- Use slightly different numbers or letter scales
- Emphasize certain features more than others
- Present reports in more or less detail
Underneath those differences, they’re all trying to do the same thing: describe how the embryos are doing so they can choose the best one(s) to try first.
If you ever move between clinics or get a second opinion, it’s normal to notice small differences in phrasing. You can always ask each team to explain their approach and how they see your specific embryos.
4. Can an embryo grade tell me what kind of child I’ll have?
No. Embryo grading looks at how an embryo appears in the lab at a very early stage. It does not:
- Predict personality or temperament
- Measure intelligence or abilities
- Decide who your child will be as a person
Those parts of the story come later, through family, environment, community and all of the experiences your child will have as they grow.
Explore Your Path to Parenthood With Joy of Life
Whether you’re just beginning to explore IVF and surrogacy or are already in treatment, embryo grading charts can raise a lot of questions. At Joy of Life, we can help you make sense of the information you’ve been given, align it with your goals and move forward with a plan that feels clear and supported.
If you’re still looking for the right partner on your path to parenthood, you can apply to become a parent with Joy of Life or contact us for a short, no-pressure conversation about your next steps.